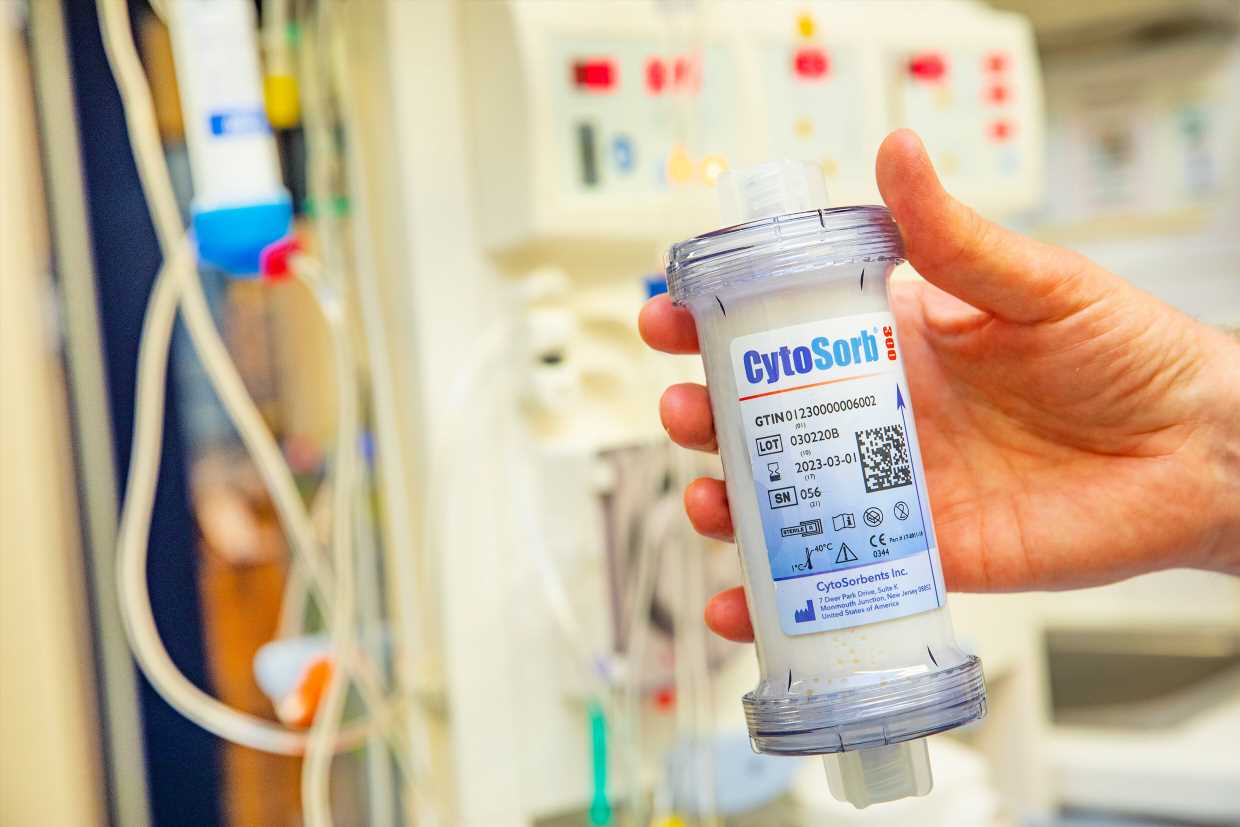
Many hospitals use the adsorber to purify the blood of seriously ill patients in order to trap inflammatory substances and prevent the life-threatening cytokine storm. MHH researchers have now found in a meta-study that the treatment does not reduce mortality and may even cause harm.
Blood purification procedures are used for a variety of diseases such as kidney failure or severe infections. The best-known form of blood purification is hemodialysis for kidney failure. There are also various treatments known as therapeutic apheresis, which ensure that pathogens or harmful metabolic products are removed from the blood.
In these procedures, which usually takes several hours, the blood is passed through a machine to remove pathogens or harmful metabolic products with the help of so-called adsorber systems. The healthy parts are then returned to the patients as an infusion.
But intensive care medicine also uses blood purification procedures to remove pro-inflammatory cytokines from the blood in cases of life-threatening excessive immune reactions caused by sepsis or COVID-19. These proteins actually control the defense against pathogens.
However, when released uncontrollably, they trigger a life-threatening overreaction of the immune system. To prevent this, many hospitals use the CytoSorb adsorber system. Used in addition to hemodialysis or on its own, the cartridge is supposed to intercept the problematic messenger substances and ensure that those affected survive the dreaded cytokine storm.
Now researchers from the Clinic for Kidney and Hypertension Diseases at the Hannover Medical School (MHH) have examined the effectiveness of the adsorber in more detail for the first time.
They analyzed data from 34 studies in which about 1,300 patients treated with CytoSorb were compared with about 1,300 control subjects. The result: “We could not find any measurable reduction in mortality due to CytoSorb treatment,” says Professor Dr. Bernhard Schmidt, senior physician at the clinic.
The use of the cartridge, which costs around 1,100 euros more, can even have negative consequences. This is because the adsorber not only removes the pro-inflammatory cytokines, but also other components of the blood plasma such as anti-inflammatory tissue hormones, coagulation factors and antibiotics.
“Therefore, we cannot recommend the use of CytoSorb in intensive care medicine,” the nephrologist states. The results of the meta-analysis have been published in the journal Critical Care.
Use increases from year to year
The adsorber is manufactured in the U.S. and has been used for eleven years in German hospitals as an additive in blood purification. The number of uses increased from year to year and was about 6,500 in 2020. The number of studies on the use of CytoSorb is also considerable. A search by the MHH researchers in the PubMed medical database yielded 410 hits, and there were about 800 in CytoSorb’s own database. But by no means were all the studies suitable for inclusion in the meta-study.
“Most of them were completely inadequate in terms of their scientific quality, had cohorts that were too small, used data from the same patients several times and compared completely different disease courses,” explains Professor Schmidt. Thirty-four studies finally remained that the nephrologist and his team reviewed. Of these, only twelve were randomized, i.e., had randomly assigned their participants to different groups, so that it was not predictable who would receive the blood purification with adsorber and who would belong to the control group.
Appropriate studies are lacking
Nevertheless, the meta-study does not exclude that CytoSorb might not have a positive effect under certain circumstances, emphasizes Professor Schmidt. “In certain patients in the very early phase of sepsis, the adsorber could possibly help,” he says. “But these are case-by-case decisions.” In order to clearly prove the effectiveness, randomized, controlled studies on suitable patients in comparable disease states are missing.
For this, however, preliminary work has to be done to find patients who are likely to respond to the treatment and to determine the optimal time for therapy for each disease, he says. After all, the meta-study is now part of the CytoSorb database. The nephrologist does not want to speculate on whether the use of the adsorber in German hospitals will decrease as a result of its publication. At the MHH, however, the cartridge has already been used less frequently for some time.
More information:
Sören Becker et al, Efficacy of CytoSorb®: a systematic review and meta-analysis, Critical Care (2023). DOI: 10.1186/s13054-023-04492-9
Journal information:
Critical Care
Source: Read Full Article