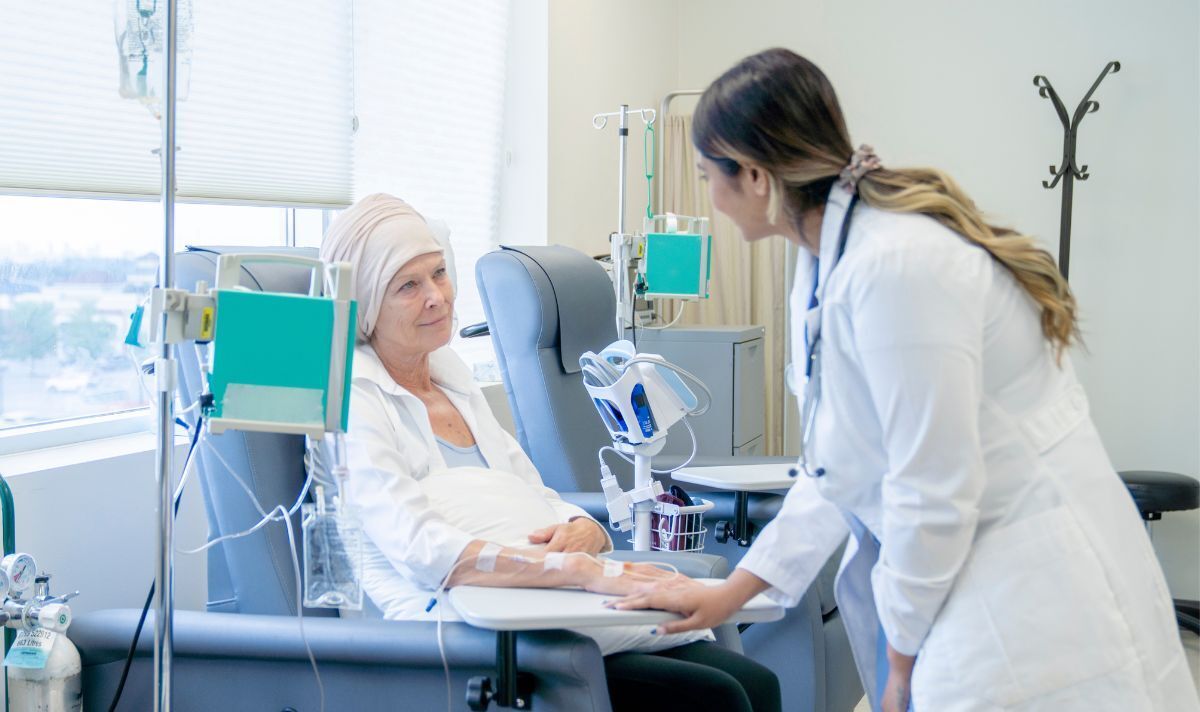
Dr Amir speaks about revolutionary new cancer test
Health services will be hit by a “silver tsunami” of older cancer patients over the next two decades, leading oncologists have warned.
An ageing population is expected to fuel a boom in more complex cases which will escalate pressure on the already stretched NHS. Experts called for urgent action to grow the medical workforce as they warned the world was “not prepared”.
Dr Andrew Chapman, director of the Sidney Kimmel Cancer Center in Philadelphia, said: “As we age, the potential to develop cancer increases.
“Because people are living longer, there’s going to be more cancer incidence which means a higher volume of people that we need to take care of and their needs are very unique.
“The point behind the silver oncologic tsunami is that as the population expands and the incidence goes way up, are we really prepared to deal with those needs? I think globally, we’re not prepared.”

The number of annual diagnoses in the UK is projected to rise by a third by 2040, surpassing half a million for the first time.
And the proportion of cases involving patients aged over 70 will rise from half now to six in 10, according to Cancer Research UK (CRUK).
Dr Chapman raised the alarm at the American Society of Clinical Oncology’s (ASCO) annual conference in Chicago this weekend, attended by 40,000 cancer doctors from across the globe.
He warned that if health systems did not prepare, patients would receive “suboptimal care” if services are overwhelmed.
He also cautioned against ageism, saying: “Sometimes there’s a nihilism – ‘if you’re older we’re not going to bother’ – which is horrible.
“Age is not that relevant. The point is how physically fit you are and not everybody the same age is the same level of fitness.”

Older patients are more likely to have other underlying health conditions which make their treatment more challenging.
They may also have different priorities when it comes to treatment, Dr Chapman said. “Most of the time, older adults care more about maintaining their function than they necessarily care about the cancer.
“They want to go to weddings, they want to see their grandkids, they want to play golf. If you’re going to give somebody treatment that’s going to take that away, they may not want it.
“Much different than somebody who’s 45 who wants to live for another 40 years. It’s a different game.”
Professor Charles Swanton, CRUK’s chief clinician, told reporters older patients often require more careful management.
“Diseases of ageing are obviously more common among 70-year-olds than in 40-year-olds,” he said. “As a result, what’s called polypharmacy [patients taking multiple medications] is a problem too.
“The question is, ‘How is the health system going to cope with that?’. We have a workforce problem now with around 384,000 cancer cases a year today, which is projected to rise to over half a million in 2040.”
Don’t miss…
Thousands of bowel cancer patients could be spared radiotherapy[LATEST]
Woman waited one year for cancer diagnosis after doctors failed to spot signs[LATEST]
Healthy young woman’s flu-like symptoms turned out to be cancer[LATEST]
We use your sign-up to provide content in ways you’ve consented to and to improve our understanding of you. This may include adverts from us and 3rd parties based on our understanding. You can unsubscribe at any time. More info
Analysis by CRUK suggests the number of annual cancer deaths is also set to climb by almost a quarter from 167,000 now to 208,000.
Chronic staff shortages in the NHS are already hindering efforts to clear backlogs and cut waiting times for cancer care.
In March – the latest month for which data is available – just 64 percent of cancer patients started treatment within two months of an urgent referral, against a target of 85 percent.
Prof Swanton said an exodus of doctors leaving was “becoming a major problem” and called for urgent action to grow the workforce.
He said: “If we’re dealing with 30 percent more cancer diagnoses, and those cancer diagnoses are more complex, we’re going to need at least 30 percent more oncologists, surgeons and pathologists to cope with the caseload.
“Given that it takes 15 years to train them, we need to start thinking about increasing medical school places now and making the health service more attractive to work in so that we can retain the staff we do train.”
Prof Swanton added: “There is an opportunity over the next year or two to be prepared. It’s not too late but we have to act quickly.
“The workforce issues are already a major challenge in the NHS, with unfilled positions in the diagnostic space and at consultant level. And that’s before we’ve had a 30 percent rise in the number of cancer diagnoses.”
Dr Julie Gralow, ASCO’s chief medical officer, said staff shortages were a global concern. She said: “Those workforce concerns become particularly pressing when you consider the growing number of older adults and the fact that cancer risk increases with age.”
More diverse clinical trials are also needed to collect data on how drugs affect older patients, Dr Gralow said. “We need to include older patients in trials so that we can understand the toxicities and efficacies of therapies on this population, as they have more comorbidities, frequent polypharmacy, decreased organ function and activity levels, differences in drug metabolism etc.”
Professor Paul Pharoah, of Cedars-Sinai Medical Center, said many studies focused on younger patients. He added: “Consequently the benefits and harms of treatments such as radiotherapy or chemotherapy are less well understood in older patients.
“Older patients are less likely to tolerate the harms of these treatments and so the benefit to harm ratio may be different.”
Caroline Abrahams, charity director at Age UK, said the NHS would need more geriatricians. She added: “The geriatrician’s skill set is particularly important because we know that many older people with cancer are managing other long term health conditions as well, and they need treatment and support that takes into account how these various problems interact in our ageing bodies.”
An NHS spokesperson said the health service was treating record numbers for cancer and rolling out new initiatives for early diagnosis.
They added: “We know we have a growing and ageing population, which inevitably increases the number of people needing NHS care and the intensity of support they require.
“As set out in the NHS Long Term Plan we are working with partners to ensure doctors are trained with the generalist skills needed to meet the needs of an ageing population, alongside the development of specialist knowledge and skill.”
A Department of Health and Social Care spokesperson said: “There are more doctors, nurses and staff working in the NHS than ever before with 50 percent more specialist cancer doctors treating patients now compared to 2010.
“The NHS is also seeing, treating and saving record numbers of people with cancer but we know there is more to do.
“That is why we are seeking views on our Major Conditions Strategy and the NHS will soon be publishing a long-term workforce plan setting out how it will recruit and retain even more staff.”
Source: Read Full Article