For our free coronavirus pandemic coverage, learn more here.
At least 2.2 million Australians have now been infected with COVID-19. Despite high rates of vaccination, breakthrough and repeat infections are occurring.
Unfortunately, the idea that we are immune from the virus once we’ve been infected, and can finally relax and return to life as “normal”, doesn’t quite hold true.
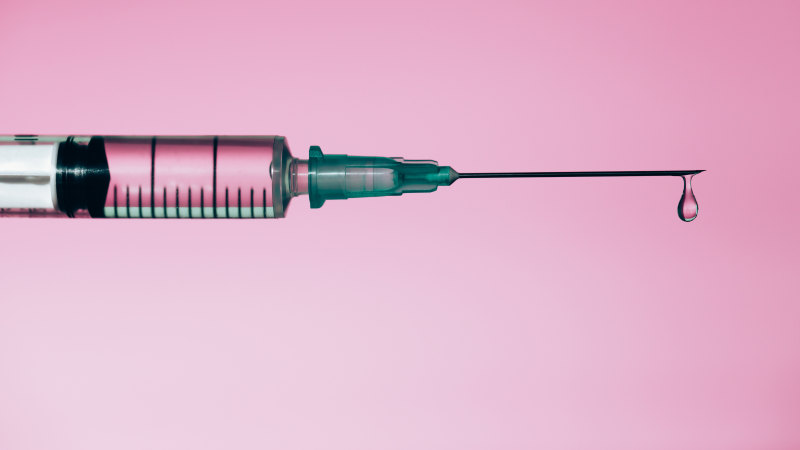
Protection, not perfection: Neither vaccines nor infection give us long-lasting immunity against COVID reinfection.Credit:Getty
So, what immunity do we have from reinfection and, how long does it last?
“It’s not a straightforward answer,” admits Professor Stuart Tangye the leader of the Immunity and Inflammation Research Theme at Garvan Institute of Medical Research.
Though infection does seem to provide some immunity, it is unclear how long that lasts and how strong that protection is. It may also vary from person to person, and variant to variant. According to NSW Health: “People who have recovered from COVID-19 have a low risk of getting it again in the 28 days after you are released [from isolation] as most people develop some immunity.”
“We really don’t have the timeline to establish how long immunity, induced by Omicron infection, lasts,” Tangye says.
Several large studies around the world have shown that infection with other variants of COVID reduces our chance of reinfection by over 90 per cent, at least initially.
“Infection does not produce long-lasting immunity,” says Dr Cassandra Berry, a professor of Viral Immunology at Murdoch University. “Antibodies will wane after a few months and are unreliable in neutralising the virus.”
The good news is that, if you do get reinfected with the same or a new variant it is much less likely to be severe.
This is because when our body encounters an infection for the first time, it activates our innate immune response – the one that launches the same response regardless of the invader – to hold the infection at bay. “Then you send in the troops… which is your adaptive immune system – the T-cells and B-cells,” Tangye says.
“We really don’t have the timeline to establish how long immunity, induced by Omicron infection, lasts.”
This whole process can take seven to 10 days. Once we have been infected – or vaccinated – however our immune system has been “supercharged” to encounter the invader and this same process only takes a couple of days.
“The biggest difference between being vaccinated and unvaccinated, or infected and reinfected is that your immune system has been trained to respond very, very quickly,” Tangye explains. “Vaccination or primary infection – presuming you survive primary infection – can put you in very good standing to have much better protection next time round whether that’s the initial virus or a variant.”
According to Berry – who is no relation to this writer – immunity from the vaccine, while not perfect, is more protective than natural immunity through infection.
This is because if we are infected with the whole virus, our body is exposed to multiple antigens (substances that cause an immune response). As our immune system tries to tackle these, it produces a number of “non-neutralising ineffective antibodies”.
“The immune response gets distracted with multiple antigens,” Berry explains. “But with vaccines delivering only the spike protein, the immune system can focus and responds to activate our B and T cells and produce anti-spike antibodies.”
This induces a kind of immune memory that activates when we are exposed to the infection again. And although the tip of the spike protein changes in each variant, the base remains the same: “If we can get antibodies that will neutralise the base of the spike, that’s our broad neutralising antibody response that can protect us across emerging variants.”
Another reason to keep up your vaccinations, according to Berry, is a reduced risk of long COVID: “Although immune responses will be restimulated there is a chance of long COVID after natural infection.”
On Tuesday, NSW Chief Health Officer Kerry Chant said people who have had COVID-19 can receive their booster four to six weeks after recovery.
If you have “hybrid immunity” – that is you have been vaccinated and had a breakthrough infection – your response against reinfection may be even stronger, says Berry, but will still not last for long.
Again, because COVID-19 has only been around for a couple of years, is evolving quickly and most of the studies looking at natural immunity have lasted several weeks or months, it’s hard to give more definitive answers.
“We don’t really have that longitudinal analysis to know how long your immunity is going to be effective and protective for,” Tangye says.
Age, underlying health conditions and certain genes can also affect our immune response and the length and strength of our immunity following infection.
As far as the impact of reinfection on transmissibility, some studies have suggested that the viral load is lower.
“That’s probably because you have antibodies and T-cells that are clearing the virus more quickly,” he explains. “So the extrapolation of that is less virus, less transmission. But vaccination or infection does not prevent transmission totally.”
For these reasons, while the experts agree you can probably “relax” temporarily because you can enjoy a brief period of protection if you have been infected (and preferably boosted), its worth remembering it only lasts a matter or months (or less for the unlucky few who are reinfected within 28 days).
Taking precautions is still important, especially around vulnerable people, and we will still need boosters every six-to-12 months.
Berry anticipates annual vaccination with a combination of Influenza HA and COVID spike antigens.
“Using different vaccine brands and types can help increase protection levels against emerging virus variants,” she adds.
Tangye says that soon, scientists will be able to engineer seasonal vaccines, based on the predicted evolution of each new variant, like they do with the annual flu vaccines.
“Its still evolving,” he says, “but, here we are two years later and 5.5 million deaths – this ain’t going anywhere fast.
“We’re probably not going to eradicate the virus entirely, but hopefully, we’ll get to the point where things are manageable.”
And the key to making it more manageable remains the same: get vaccinated and get boosted, even if you’ve been infected, he says: “That’s really, really key to all of this.”
Make the most of your health, relationships, fitness and nutrition with our Live Well newsletter. Get it in your inbox every Monday.
Most Viewed in Lifestyle
From our partners
Source: Read Full Article